Unlocking the Gut-Skin Connection: A Holistic Approach to Functional Skin Disorders
Have you ever felt uncomfortable in your own skin? You may think to yourself, “If only this rash or acne will go away, THEN I will feel confident.” Maybe you have tried various topical creams, been prescribed antibiotics, or purchased the “next best thing” to help cure those blemishes. (Let’s be honest … we have ALL been there at one point or another.)
I have worked with COUNTLESS clients who come to me with skin concerns, whether it be acne, rosacea, psoriasis, or eczema. Most of them have been struggling with these problems for YEARS, and have tried all of the various “solutions” listed above. What most people don’t realize is that there is a bigger issue lying within the body that needs to be addressed. That issue is your gut.
Understanding the Gut-Skin Connection
The skin is our body’s largest organ and plays many important roles for our body. It is made up of many layers, many of which we can’t see. The skin barrier serves as our body’s first line of defense. If this outermost layer becomes damaged, bacteria, free radicals, and toxins can sneak past and wreak havoc inside our bodies.
If too many of these pathogens push past the barrier, this can lead to inflammation not only on the outside of the skin, but also throughout the body, including the gut. Think of skin as the outward “checkpoint” of gut health. If there are any imbalances in the gut, guess where one of the first places is for the imbalances to show up? You’ve guessed it … the skin!
How Does Gut Health Impact Skin Disorders?
It is estimated that the gut makes up more than 70% of the immune system. Gut imbalances can manifest on our skin due to the Gut-Skin Connection.
The Gut-Skin Connection refers to the two-way communication system between the gut microbiome and the skin. The gut microbiome is constantly communicating with the skin on aspects such as inflammation, skin structure, and sebum production.¹ Sebum is the oily material on the skin’s surface. With gut imbalances, such as leaky gut, gut dysbiosis, or gut pathogens, skin will be negatively impacted.
Take acne, for example. Acne is one of the most prevalent skin issues and has been linked to gut inflammation and bacterial overgrowth. Rosacea, another common skin issue, is most oftentimes caused by gut dysbiosis. These are just a few of the common skin disorders we encounter at my functional medicine practice. Lifestyle plays a major role in skin disorders, but using lab testing to take a deeper look at what is going on internally can also be helpful. Let’s dive into these skin conditions, as well as a few more, below.
3 Common Skin Disorders: Why Gut Health Matters
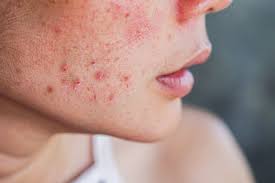
1. Acne
Acne is one of the most prevalent conditions in America. Not only do an estimated 95% of teens suffer from acne, but also over half of American adults do, too.² Although this skin condition varies by type and severity, acne has been linked to multiple gut issues.
Your gut is partly responsible for fatty acids composition, which are a part of sebum. If sebum production is imbalanced, this can lead to acne. Interestingly enough, one Russian study found over half of study participants with acne had major disruptions to their gut flora, also known as gut dysbiosis.³
In addition, leaky gut (aka intestinal permeability) also has a connection with acne. Leaky gut refers to holes or gaps in the intestinal lining that cause bacteria to “leak” into the body. This can lead to inflammation and several GI-related symptoms. If these bacteria make their way into the gut, this also affects the gut microbiome’s communication with the skin, which can show up as acne for many people.⁴ Before we dive into some sustainable lifestyle tips and tricks, let’s talk about eczema next.
2. Eczema
Eczema is commonly characterized by dry, inflamed, itchy skin caused by damage to the skin barrier. It is estimated that over 30 million Americans currently suffer from eczema.⁵ This skin disorder is unique in that there is a direct relationship with the immune system, although the underlying cause could be from a multitude of factors. For one, food allergies and food sensitivities could contribute to or worsen eczema prevalence in infants and children. This can even carry on into adulthood.⁶
Although research is ongoing, there have been several potential links to gut imbalances and leaky gut. One research study analyzed children with atophic eczema, a common form of eczema, and found they had a higher rate of intestinal permeability than those without this skin disorder.⁷ An additional study found those with another type of eczema, seborrheic dermatitis, had abnormal gut flora compared to healthy control participants.⁸
Interestingly enough, there has also been a genetic link discovered with eczema. One particular gene, the FLG gene, has been found to be defective in about 70% of those diagnosed with this skin condition.⁶ This gene plays a role in producing cells to make the skin’s outermost layer. If this gene is defective, it can have a negative impact on the skin barrier, thus increasing the risk for developing eczema flare-ups.
Eczema can have a negative impact on a person’s quality of life. Functional lab testing can be beneficial and the lifestyle approaches discussed later in this article can help manage eczema flare-ups and significantly improve quality of life.
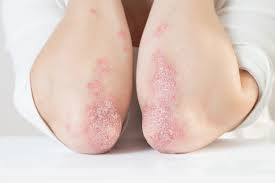
3. Psoriasis
Psoriasis is defined as raised areas of skin patches that are typically red or purple in color and can leave skin looking dry, scaly, and itchy. This autoimmune skin disorder impacts both males and females equally. Furthermore, it is estimated that over 7 million Americans currently have psoriasis.⁹
Like eczema, this skin condition also has an immune connection. Current research shows that those with psoriasis tend to have a disrupted gut microbiome, along with significant gut inflammation, commonly caused by leaky gut.¹⁰ In addition, there has been a potential link between Crohn’s disease, a type of inflammatory bowel disease (IBD), and psoriasis. Those with Chron’s may develop plaques similar to psoriasis. Fortunately, similar treatment methods can be used for the two conditions.¹¹
There have also been several pathogens identified as potential triggers for psoriasis. These include the bacterial strains Staphylococcus aureus, Streptococcus bacteria, and Helicobacter pylori (H. pylori), along with the fungi Candida and Malassezia.¹² Through functional lab testing, it is possible to identify these potential pathogens, along with any leaky gut or gut dysbiosis.
Now that we have gone through the basics of three common skin disorders, let’s dive into some lifestyle approaches that can help!
Lifestyle Modifications for Functional Skin Disorders
Stress Management
Not surprisingly, stress not only has a role in the gut, thyroid, and other major organs, but it also plays a role in skin health. Prolonged stress can have a negative impact on the gut and digestion, but it can also upregulate the immune response in the body. This heightened, unnecessary immune response can eventually send upregulated signals to the skin, causing one of many skin conditions.
Stress can be internal or external. Internal stress refers to things going on inside the body, whether it be leaky gut, gut dysbiosis, or another imbalanced body system. External stress refers to things going on in the world around us, including emotional stressors or dietary stressors.
Stress management through daily mindfulness practices is critical. Whether it be deep breathing, journaling, meditation, or reading, consistent mindfulness has been shown to lower internal stress levels. It helps to keep the adrenal glands in check and manage our nervous system response.
Sleep Quality
Let’s be honest: most of us are not consistent with our sleep routines (also known as sleep-wake cycles). In fact, it is estimated that 1 in 3 American adults are constantly sleep deprived13. In addition, about half of American adults report not getting enough sleep and feeling tired at least three days of the week.¹³
These disruptions to our Circadian Rhythm cues can have a major impact on our daily lives. Over time, they can lead to increased risk for developing certain chronic health conditions, such as obesity, type 2 diabetes, and certain cancers.
Overall Diet Quality
Diet quality plays a huge role not only with our digestion and risk for various chronic diseases, but also our mood. The Standard American Diet (SAD) is full of processed foods and lacks the nutrient variety that our body needs. In fact, multiple studies have studied the impact of the American
Diet quality plays a huge role not only with our digestion and risk for various chronic diseases, but also our mood. The Standard American Diet (SAD) is full of processed foods and lacks the nutrient variety that our bodies need.
In fact, multiple studies have researched the impact of the American diet on skin health. For example, an Integrative Dermatology article analyzed specific nutrition modifications, including a whole foods diet, which can have positive improvements on skin disorders.¹⁴ Additionally, supporting gut health through probiotics has been shown to increase outcomes. Probiotics, the beneficial gut microbes, can have a major impact on skin health. Proposed benefits include reduced inflammation and oxidative stress, thus improving skin quality.¹⁵ Specific strains can be targeted to treat certain skin conditions. For example, Bifidobacteria has been shown to improve eczema in one study’s participants.¹⁶
Functional Medicine and Functional Lab Testing For Skin Disorders
Along with lifestyle approaches, functional lab testing can provide specific next steps to take to improve skin outcomes through analyzing specific markers, including gut health. In summary, eating a wide variety of whole foods, managing stress, and promoting adequate sleep all work together to achieve an overall healthy lifestyle.
Please note: This article is not intended to be medical advice, nor is it meant to treat, diagnose, or cure any injury or illness. It is for informational purposes only.
To book a FREE 30-minute root cause analysis with functional lab testing click here!
References:
- Salem I, Ramser A, Isham N, Ghannoum MA. The Gut Microbiome as a Major Regulator of the Gut-Skin Axis. Front Microbiol. 2018;9:1459. Published 2018 Jul 10. doi:10.3389/fmicb.2018.01459
- https://www.rupahealth.com/post/a-functional-medicine-approach-to-cystic-acne
- Volkova LA, Khalif IL, Kabanova IN. Vliiane disbakterioza kishechnika na techenie vul’garnykh ugreĭ [Impact of the impaired intestinal microflora on the course of acne vulgaris]. Klin Med (Mosk). 2001;79(6):39-41.
- Omenetti S, Pizarro TT. The Treg/Th17 Axis: A Dynamic Balance Regulated by the Gut Microbiome. Front Immunol. 2015;6:639. Published 2015 Dec 17. doi:10.3389/fimmu.2015.00639
- https://nationaleczema.org/research/eczema-facts/
- https://www.rupahealth.com/post/a-functional-medicine-approach-to-eczema
- Pike MG, Heddle RJ, Boulton P, Turner MW, Atherton DJ. Increased intestinal permeability in atopic eczema. J Invest Dermatol. 1986;86(2):101-104. doi:10.1111/1523-1747.ep12284035
- Bowe WP, Logan AC. Acne vulgaris, probiotics and the gut-brain-skin axis – back to the future?. Gut Pathog. 2011;3(1):1. Published 2011 Jan 31. doi:10.1186/1757-4749-3-1
- Armstrong AW, Mehta MD, Schupp CW, Gondo GC, Bell SJ, Griffiths CEM. Psoriasis Prevalence in Adults in the United States. JAMA Dermatol. 2021;157(8):940-946. doi:10.1001/jamadermatol.2021.2007
- Visser MJE, Kell DB, Pretorius E. Bacterial Dysbiosis and Translocation in Psoriasis Vulgaris. Front Cell Infect Microbiol. 2019;9:7. Published 2019 Feb 4. doi:10.3389/fcimb.2019.00007
- Feagan BG, Sandborn WJ, Gasink C, et al. Ustekinumab as Induction and Maintenance Therapy for Crohn’s Disease. N Engl J Med. 2016;375(20):1946-1960. doi:10.1056/NEJMoa1602773
- Teng Y, Xie W, Tao X, et al. Infection-provoked psoriasis: Induced or aggravated (Review). Exp Ther Med. 2021;21(6):567. doi:10.3892/etm.2021.9999
- https://www.sleepfoundation.org/how-sleep-works/sleep-facts-statistics
- Tirant M, Lotti T, Gianfaldoni S, Tchernev G, Wollina U, Bayer P. Integrative Dermatology – The Use of Herbals and Nutritional Supplements to Treat Dermatological Conditions. Open Access Maced J Med Sci. 2018;6(1):185-202. Published 2018 Jan 21. doi:10.3889/oamjms.2018.041
- https://chriskresser.com/gut-health-and-skin-connection/
- Marras L, Caputo M, Bisicchia S, et al. The Role of Bifidobacteria in Predictive and Preventive Medicine: A Focus on Eczema and Hypercholesterolemia. Microorganisms. 2021;9(4):836. Published 2021 Apr 14. doi:10.3390/microorganisms9040836

Rachel Scheer is a Certified Nutritionist who received her degree from Baylor University in Nutrition Science and Dietetics. Rachel has her own private nutrition and counseling practice located in McKinney, Texas. Rachel has helped clients with a wide range of nutritional needs enhance their athletic performance, improve their physical and mental health, and make positive lifelong eating and exercise behavior changes.
Read This Next
Micronutrients, or the vitamins and minerals your body needs, typically work like a team. To…
If you want to improve gut health, or even optimize your overall health, you’ve probably…
Have you ever found yourself grappling with the discomfort of abdominal distension, bloating, or cramping,…